Degenerative Disc Disease
Make an Appointment
Consult Dr. Loo Wee Lim
What is Degenerative Disc Disease?
Degenerative disc disease is very common as one ages. They can cause low back pain, leg numbness, leg weakness and inability to walk far distances without stopping.
Xray and MRI are commonly done for further evaluation if the symptoms are not relieved with rest and painkiller.
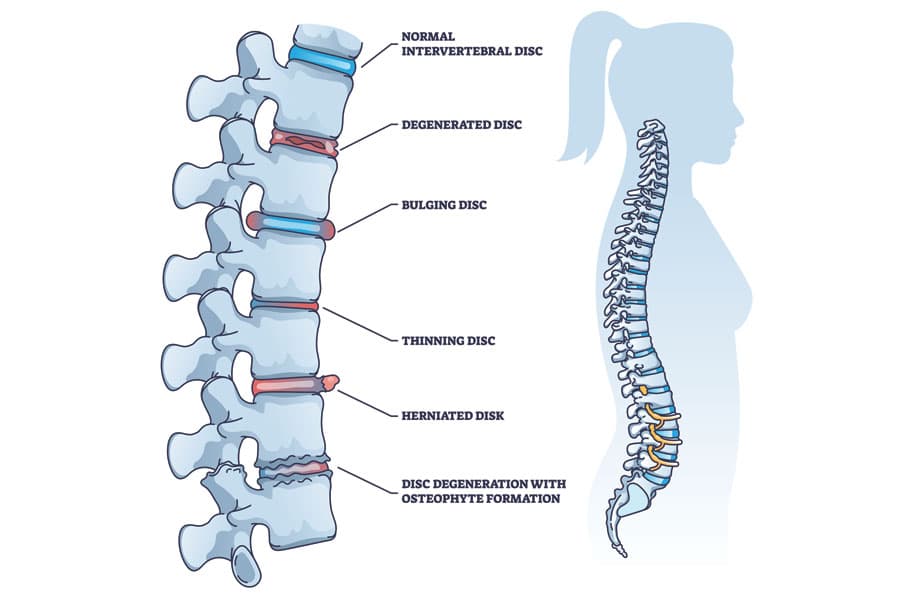
Spinal discs are rubbery cushions between your vertebrae which are the bones in your spinal column. The discs function as shock absorbers that are important for the body to move, bend and twist comfortably.
Our spinal discs degenerate over time due to repeated daily stresses on the spine and it happens to all of us as we age.
Main Causes of Degenerative Disc Disease?
Dry Out
is a age-related degenerative condition. At birth, our disc consists of 80 percent water. The disc eventually dries out and does not absorb shock as efficiently.
Sporting Activities
can cause tears in the outer core of the disc. Generally, most people will have some degree of disc degeneration by age 60 or older.
Injuries
that can cause inflammation, soreness and instability. Repeated injuries are often a leading cause of back pain.

Frequently Asked Questions
The most obvious symptom of degenerative disc disease is a mild, persistent pain around the degenerative disc that occasionally flares up into a more chronic and potentially debilitating pain.
A combination of physical therapy and pain medication can offer long-term relief from symptoms caused by degenerative disc disease.
Through physical therapy and rehabilitating exercises, you can strengthen the muscles in your neck and back to better support your spine. This will help greatly to alleviates your back pain while also improving your posture and flexibility.
Your doctor may use imaging tools such as X-rays, CT scans, or MRI to check the condition and alignment of your disks. This may be followed by a physical exam to evaluate the extent of your back pain.
Your doctor may then check your nerve function by using a reflex hammer. Having little or no reaction could indicate damaged or compressed nerves. They may also test your muscle strength to check for any unusual muscle weakness or shrinking. These are all signs which could indicate nerve damage or degenerated discs.
Targeted Procedures
MIS TLIF
The goal of this procedure is to stabilise the spine, minimising low back and leg pain. This procedure stops the motion of the affected disc level by placing screws, rods and bone graft to promote the two vertebrae to become one bone (spinal fusion).
Typically two 2-3 cm incisions are made on either side of the lumbar spine. After the incisions are made, a minimally invasive approach is made down to the vertebral body using dilating tubes. The surgeon then ensures that spinal screws are securely placed into the vertebral body of spine. Live x-ray and live nerve monitoring are used to ensure that the screws are placed accurately.
Artificial Cervical Disc Replacement
A goal of this procedure is to relieve the pain caused by pinched nerves due to a damaged disc in the cervical spine. The diseased or damaged disc will be replaced with a specialised implant.
The surgeon creates a small incision in the front of the neck to gain access to the spine. The diseased disc is removed from between the vertebral bodies.
The surfaces of the vertebral bodies are cleared of all damaged disc tissue and shaped to accept the implant.
The artificial disc is inserted into the space between the vertebrae and carefully tapped into place. The endplates are designed to bond tightly to the vertebral bodies, stabilising the spine.
ACDF
An ACDF is done with an anterior approach, this means that the surgery is done through the front of the neck and not through the back of the neck. This approach has several typical benefits which includes allowing the surgeon direct access to the disc and less post-operative pain.