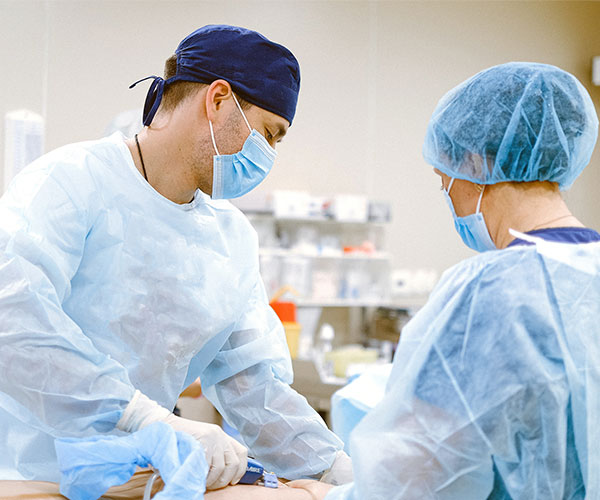
Herniated Disc (Slipped Disc)
What is a Herniated Disc?

An herniated disc can be extremely distressing and painful. It can cause permanent numbness and weakness if left untreated. Early diagnosis and treatment allows earlier return to function and prevents nerve damage.
A Discectomy (removal of herniated disc) can be performed by the open technique, minimally invasive keyhole technique or via endoscopy. Most patients can be discharged within 24-48 hours after the procedure.
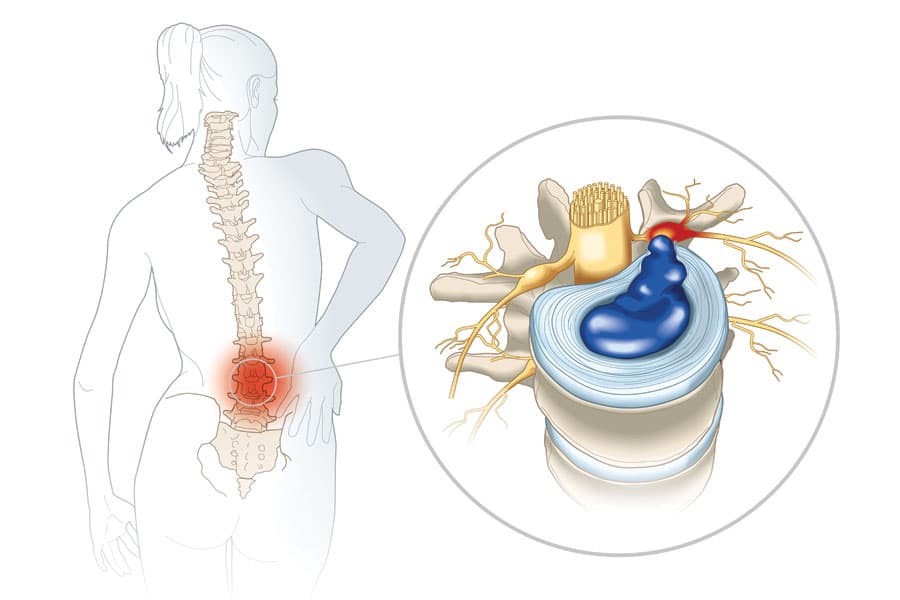
A single excessive strain or injury may cause a herniated disc. Additionally, disc material also tend to degenerate as part of the natural aging process.
Eventually, the ligaments that hold a disc in place begin to weaken. When this degeneration process is left unchecked, a minor strain or twisting movement can cause a disc to rupture.
Types of Spinal Surgery
removes part of the bone around a herniated disk and expand the spinal canal.
replaces a damaged herniated disc with an artificial one.
directly joins two or more vertebrae to stablise your spine.
is a minimally invasive technique that is used to remove the herniated portion of intervertebral disc.
Frequently Asked Questions
Symptoms can vary greatly, it often depends on the position of the herniated disc as well as the size of the herniation. If the herniated disc is not pressing on a nerve, you may experience a slight pain in your back or even no pain at all. However, if the disc is pressing on a nerve, there may usually be pain, numbness or weakness in the area which the pressed nerve is located.
For lumbar and cervical herniated discs, non-surgical treatment options can usually be applied to help alleviate any pain and discomfort (4-6 weeks). Patients may try non-surgical treatment to assess if further treatment options (including surgery) may be needed.
The benefits of surgery should be weighed carefully against its risks. Despite a large percentage of patients with herniated discs reporting considerable pain relief after surgery, it does not always guarantee a successful outcome.
A patient may consider spinal surgery if there is:
- Constant pain that negatively affects quality of life
- Development of neurological issues such as leg weakness and/or numbness
- Difficulty in standing or walking
- Loss of normal bowel and bladder functions
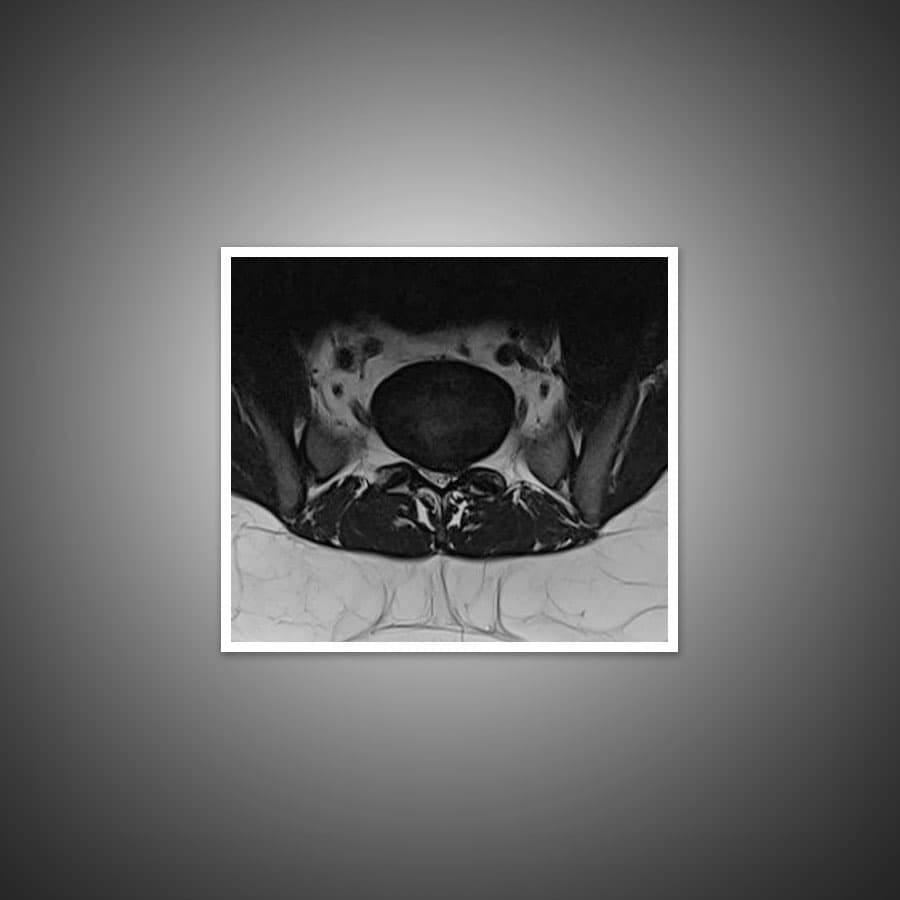
The most common imaging for herniated disc is MRI. X-rays of the affected region are usually added to get a better evaluation of the vertebra. CT scan and myelogram will only be ordered if the initial scans using MRI and X-rays are inconclusive in helping to form a clear diagnosis.
Targeted Procedures
Lumbar Disc Microsurgery
This minimally invasive technique is used to remove the herniated portion of intervertebral disc. It is 95-98% effective in eliminating leg pain (sciatica) caused by nerve root compression. The procedure is performed through a small incision on the back.
The procedure usually involves:
- 1) Lamina opening: after creating small incision directly over the herniated disc, the surgeon creates a small window in the lamina (the bone covering the spinal canal). The pinched nerve roor and the herniated disc can been seen through this opening.
- 2) Spinal nerve moved: the surgeon uses a nerve retractor to gently move the spinal nerve away from the herniated disc.
- 3) Herniation removed: The herniated portion of the disc is removed, eliminating pressure on the nerve root. Only the damaged portion of the disc is removed, leaving any healthy disc material to retain its function as a shock absorber between the vertebrae.
Lumbar Epidural Steroid Injection
This injection procedure is performed to relieve low back and radiating leg pain. Steroid medication can reduce the swelling and inflammation caused by spinal conditions.
The procedural steps are:
- 1) The patient lays face down. A cushion under the stomach area provides comfort and flexes the back. A fluoroscope assists the doctor in locating the appropriate lumbar vertebrae and nerve root. A local anaesthetic is used the numb the skin.
- 2) Using the fluoroscope for guidance, the needle is carefully advanced towards the epidural space.
- 3) A contrast solution is injected to confirm the correct location of the needle tip.
- 4) A steroid-painkiller mix is injected into the epidural space, bathing the painful nerve root with soothing medication.
MIS TLIF
The goal of this procedure is to stabilise the spine, minimising low back and leg pain. This procedure stops the motion of the affected disc level by placing screws, rods and bone graft to promote the two vertebrae to become one bone (spinal fusion).
Typically two 2-3 cm incisions are made on either side of the lumbar spine. After the incisions are made, a minimally invasive approach is made down to the vertebral body using dilating tubes. The surgeon then ensures that spinal screws are securely placed into the vertebral body of spine. Live x-ray and live nerve monitoring are used to ensure that the screws are placed accurately.