Radiculopathy
Make an Appointment
Consult Dr. Loo Wee Lim
What is Radiculopathy?

Radiculopathy refers to shooting pain down the upper or limbs. Usually they are caused by slipped disc. If the pain does not resolve with painkiller and rest, surgery may be required to remove the slipped disc.
Radiculopathy often occurs with aging. As the body starts to age, the discs in the spine begin to degenerate and can result in the discs bulging. They can also begin to dry out and stiffen.
Usually improving your posture, over-the-counter medicine or physical therapy exercises are the only treatments you will need to relieve radiculopathy symptoms.
In fact, there are cases where the symptoms of radiculopathy get better over time and do not require treatment.
Types of Radiculopathy
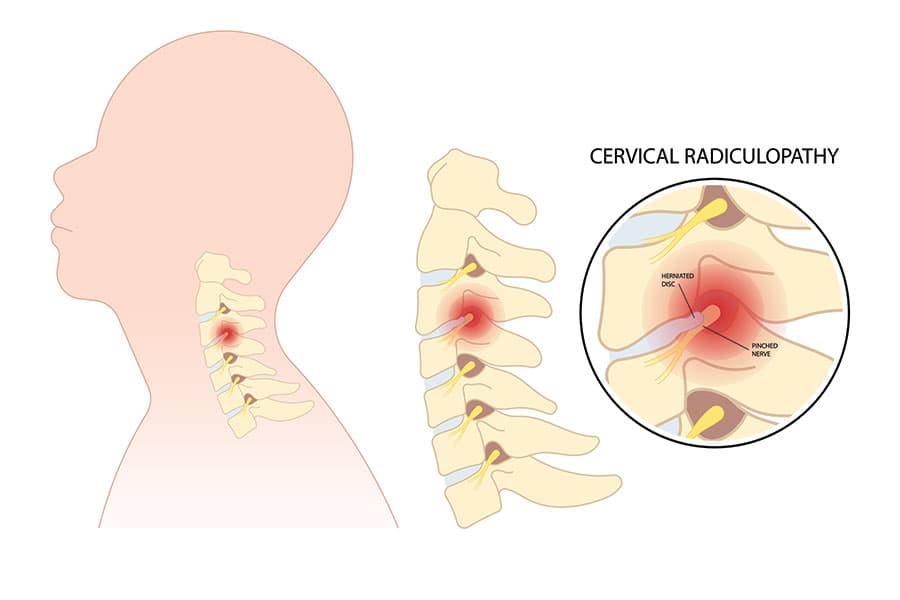
Cervical radiculopathy
This occurs when a nerve in the neck is compressed at the point where it exits the spinal cord. It may cause pain in the shoulders, as well as muscle weakness and numbness that travels down the arm into the hand.
Lumbar radiculopathy
Lumbar radiculopathy occurs in the lower region of the spine and is associated with sciatica pain. The lower back is the most common area affected by radiculopathy.
Thoracic radiculopathy
Thoracic radiculopathy is a pinched nerve that occurs in the upper region of the back, causing symptoms such as tingling, pain and numbness that can extend to the front of the body.
Frequently Asked Questions
Cervical radiculopathy can cause pain often described as burning or sharp, starting from the neck and moving to other parts of the body that are linked to the damaged nerve.
Symptoms of radiculopathy include:
- Pain in the area around your affected nerve, especially when straining your neck.
- Tingling or numbness in fingers or hand.
- Decreased motor skills.
- Loss of sensation.
There are cases where the symptoms of radiculopathy can get better after a certain curation and do not require treatment. However, if pain or other symptoms persist, your doctor will usually recommend a surgical procedure based on your symptoms and the location of your affected nerve root.
A thorough physical exam and a medical history review are usually the first steps in diagnosing radiculopathy. Your doctor will check for numbness or loss of feeling, your muscles reflexes and strength as well as your posture (i.e. abnormal spine curvature).
Other tests may include:
- X-rays to evaluate the alignment of the bones along your neck to determine any disc irregularity or damage.
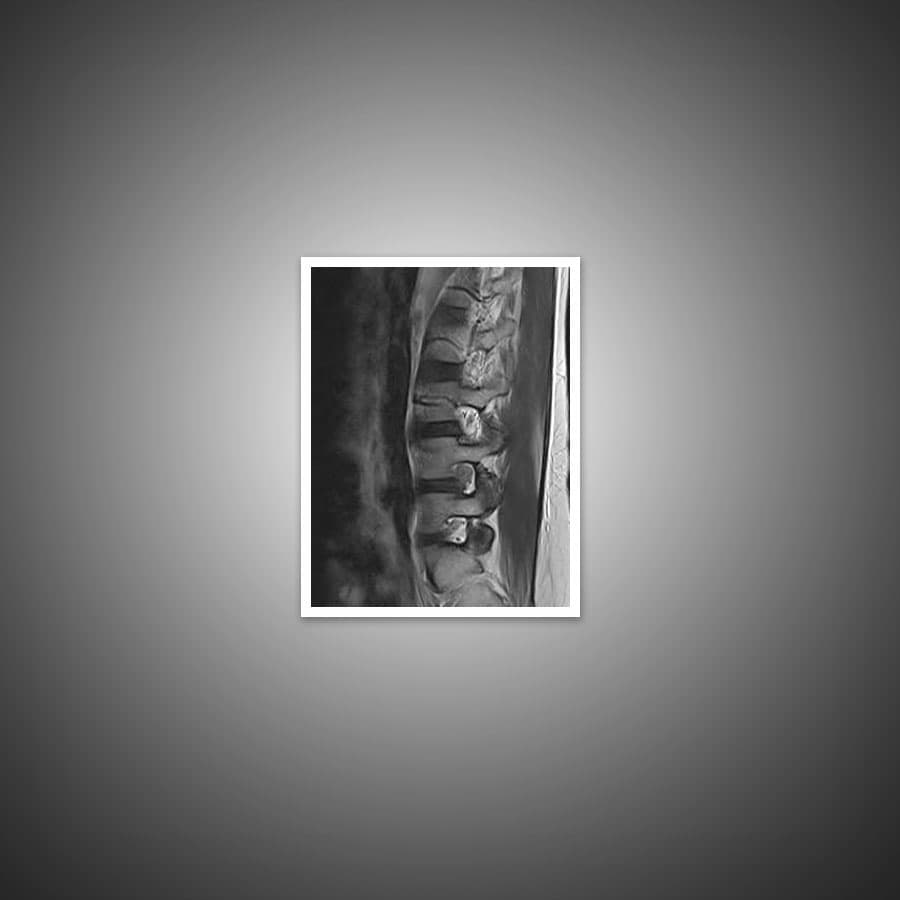
- A MRI or CT scan to find any bone spurs and herniated discs that may be pressing on the spine.
- Electromyogram to pinpoint the exact nerve root that is affected.
Targeted Procedures
Lumbar Disc Microsurgery
This minimally invasive technique is used to remove the herniated portion of intervertebral disc. It is 95-98% effective in eliminating leg pain (sciatica) caused by nerve root compression. The procedure is performed through a small incision on the back.
The procedure usually involves:
- 1) Lamina opening: after creating small incision directly over the herniated disc, the surgeon creates a small window in the lamina (the bone covering the spinal canal). The pinched nerve roor and the herniated disc can been seen through this opening.
- 2) Spinal nerve moved: the surgeon uses a nerve retractor to gently move the spinal nerve away from the herniated disc.
- 3) Herniation removed: The herniated portion of the disc is removed, eliminating pressure on the nerve root. Only the damaged portion of the disc is removed, leaving any healthy disc material to retain its function as a shock absorber between the vertebrae.
Lumbar Epidural Steroid Injection
This injection procedure is performed to relieve low back and radiating leg pain. Steroid medication can reduce the swelling and inflammation caused by spinal conditions.
The procedural steps are:
- 1) The patient lays face down. A cushion under the stomach area provides comfort and flexes the back. A fluoroscope assists the doctor in locating the appropriate lumbar vertebrae and nerve root. A local anaesthetic is used the numb the skin.
- 2) Using the fluoroscope for guidance, the needle is carefully advanced towards the epidural space.
- 3) A contrast solution is injected to confirm the correct location of the needle tip.
- 4) A steroid-painkiller mix is injected into the epidural space, bathing the painful nerve root with soothing medication.
Artificial Cervical Disc Replacement
A goal of this procedure is to relieve the pain caused by pinched nerves due to a damaged disc in the cervical spine. The diseased or damaged disc will be replaced with a specialised implant.
The surgeon creates a small incision in the front of the neck to gain access to the spine. The diseased disc is removed from between the vertebral bodies.
The surfaces of the vertebral bodies are cleared of all damaged disc tissue and shaped to accept the implant.
The artificial disc is inserted into the space between the vertebrae and carefully tapped into place. The endplates are designed to bond tightly to the vertebral bodies, stabilising the spine.
ACDF
An ACDF is done with an anterior approach, this means that the surgery is done through the front of the neck and not through the back of the neck. This approach has several typical benefits which includes allowing the surgeon direct access to the disc and less post-operative pain.